In 2018, expecting parents Dan and Lisa Callow counted down until they could welcome their first and only child, Carter, into the world. During their routine 20-week ultrasound, Lisa’s doctor noticed something alarming.
“Our local doctor knew there was something wrong, but they didn’t know what they were looking at,” Lisa explained.
The couple received a referral to the Midwest Fetal Care Center (MWFCC), a collaboration between Allina Health and Children’s Minnesota. There, a multi-disciplinary team of highly trained maternal-fetal medicine experts diagnosed the Callow’s unborn child with hydrocephalus. Hydrocephalus is a buildup of cerebrospinal fluid in the hollow places inside the brain, called ventricles, that can put a dangerous amount of pressure on a child’s developing brain.
“It scared us and terrified us,” Dan recalled about when he and Lisa got the initial diagnosis. “Knowing it wasn’t the end of the world and knowing these specialists do this all the time was comforting.”
The Callows got to work with their new care team that included Dr. Kyle Halvorson, a pediatric neurosurgeon at Children’s Minnesota, and also Dr. Saul Snowise, maternal-fetal medicine specialist at the MWFCC.
“The team told us while there is no cure for hydrocephalus, there is a procedure that they’ve been using for 70 years – meeting with the specialists really helped reassure us,” Dan said.
The couple also met with a Children’s Minnesota genetic counselor to see if that team could discover any hereditary reasons for this diagnosis – tests didn’t reveal any.
“Sometimes lighting just strikes,” Dan said about the cause of his unborn child’s diagnosis.
Carter’s care
Ultrasounds would continue to show the extent of Carter’s condition.
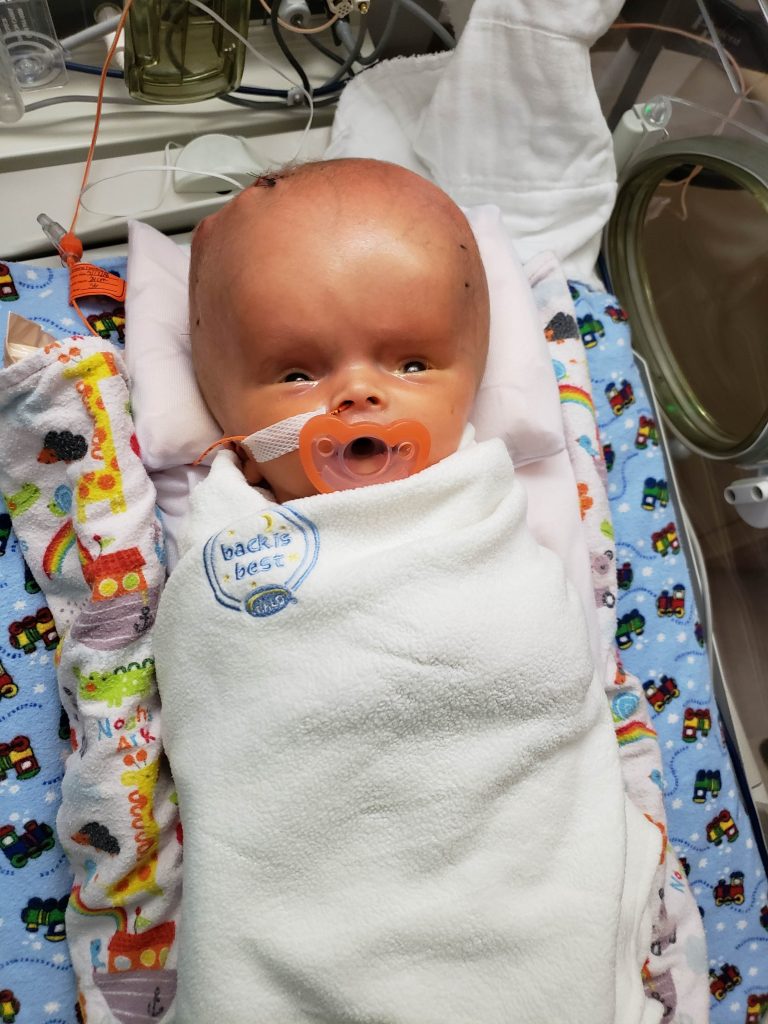
“His head was almost as big as the rest of his body during the ultrasounds,” Dan said.
The Callows and their care team prepped, monitored and waited until 37 weeks into Lisa’s pregnancy when she was considered full-term to safely deliver baby Carter via C-section.
“I wanted to meet our baby, once he was born there was something they could do for him,” Lisa said. “Once he was born we could give him to the doctors and get him the help he needed.”
Baby Carter was born on May 14, 2018, at The Mother Baby Center in Minneapolis weighing 9 pounds and 5 ounces.
“Most of that weight was his head, his body was tiny,” Lisa recalled.
Carter’s care journey was just beginning.
The first of many procedures
Just one day after baby Carter entered the world, his care team performed what would be the first of 13 surgeries during the first 13 months of his young life. Following the care plan, Carter’s neurosurgeon placed a special tube, called a shunt, from the newborn’s brain’s ventricles to the space inside his belly where the stomach and the bowels sit called the peritoneal cavity. The tube placed under Carter’s skin allows the extra cerebrospinal fluid to be absorbed into his bloodstream.
Carter would spend about seven weeks combined recovering and growing in Children’s Minnesota’s neonatal intensive care unit (NICU) and Infant Care Center in Minneapolis. He eventually went home with a feeding tube. But, Carter would undergo multiple shunt replacement procedures before his third birthday due to challenges with the amount of fluid still draining from his brain and his continued head growth. As a 2-year-old, his head size measured in the 50th percentile of a 16-year-old.
“At this point, Carter’s brain was 75%-90% just fluid, his brain was always squished because there was so much fluid in there,” Dan said. “It was a sea a fluid and very little brain.”
A new care option
Around the time Carter turned 3, Dr. Robert Tibesar, a pediatric craniofacial surgeon at Children’s Minnesota, joined his care team. Dr. Tibesar developed a cutting-edge plan to stabilize the amount of fluid in the boy’s brain once and for all. A surgery, called a reduction cranioplasty, would reduce the size of Carter’s head by half. Usually this procedure requires at least two major surgeries, but Dr. Tibesar and his team established a goal to safely complete Carter’s repair with just one. First, Dr. Tibesar and his team took a CAT scan of Carter’s skull and brain to map out the anatomy. He then conducted multiple virtual surgical planning meetings to try various surgical options and determine the best procedure for Carter and confirm it could be done safely during one surgery. This unique operation was the first of its kind in the state of Minnesota and one of only a few safely performed in the United States.
“Dr. Tibesar was very confident that he could do the surgery safety and told us he would stop if it wouldn’t be safe to do so,” Dan explained.
In November 2021, Dr. Tibesar and his team performed the eight-hour cranial vault repair procedure. There, the surgeons carefully reduced the bone mass of Carter’s head and reshaped his skull. Carter’s dad explained how a temporary drain was also placed during the procedure. Shortly after Carter’s surgery, an MRI revealed he had a minor stroke due to the pressure in his brain. After around five weeks of recovering from the stroke, Carter’s parents say their son’s care team performed another procedure to place a new shunt in his brain.
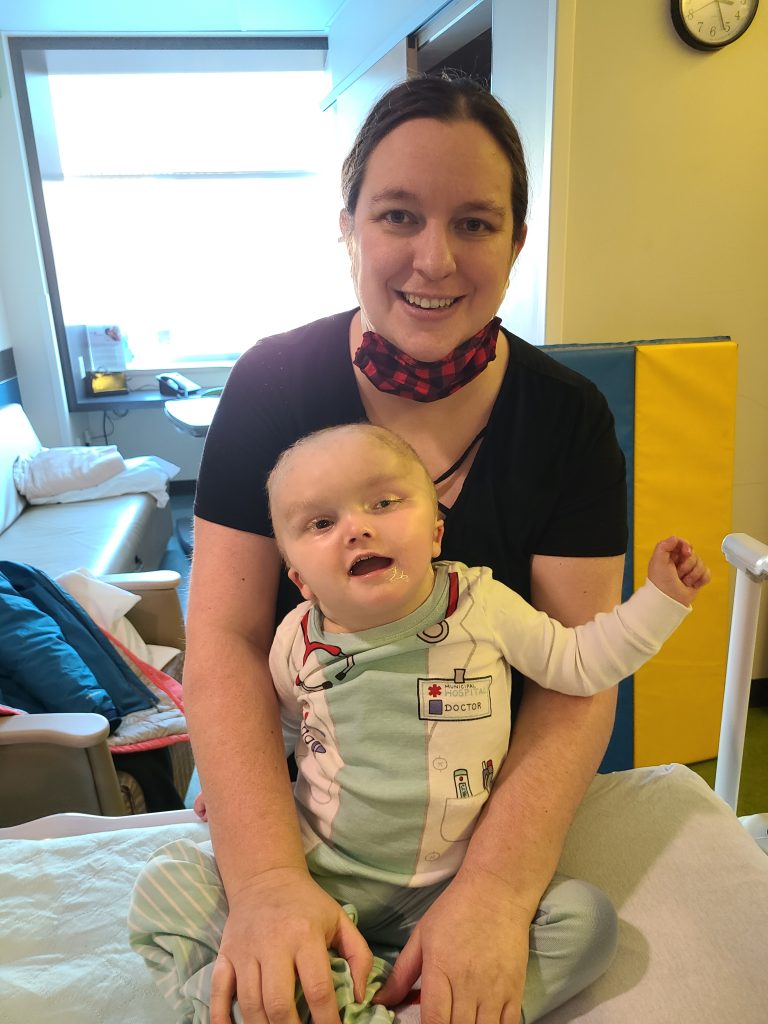
A few weeks after Carter’s procedure, his parents saw him smiling again. He can now prop himself up and play with his toys – something he wasn’t able to do by himself before the surgery.
“We are very happy we did the procedure and would still make the decision to do that procedure today,” Dan said.
Carter’s continued care
As of the summer of 2023, Carter’s head growth has stabilized after his cranial vault repair procedure, and the shunt placed during the time around that 2021 surgery has worked. Carter takes medication to control minor seizures and he also undergoes both physical and occupational therapy.
His care team has expanded to include The Kid Experts® from Children’s Minnesota’s pulmonology and endocrinology teams to help him grow in height. Carter started kindergarten in a special needs program in the fall of 2023.

“We were like, ‘OK he’s got this,’” Lisa recalled as she passed along this encouraging advice to families facing a similar diagnosis as Carter. “There’s always hope, Children’s Minnesota’s doctors – they’ve seen a lot and know what they’re doing […] they’ll get you where you need to go. Do not lose hope.”